Patient Story- Lauren

“Now, I look at my daughter and have to pinch myself. I can’t believe she’s here!”
We know the holidays can be a challenging time for many of our patients. However, today we want to share Lauren’s story with you. This time last year, Lauren wondered if she would ever become a mother. Today, she has a beautiful baby girl. Unhappy with her previous clinic, Lauren came to Dr. Miller. He listened to her concerns and together they came up with a treatment plan. Another example of how important it is to advocate for yourself when it comes to your health.
Lauren writes:
My story is one of finding hope with Dr. Miller and with the wonderful staff at the Advanced IVF Institute. My husband and I had been through a lot by the time I made a teary phone call to the receptionist (or angel?) at Dr. Miller’s office. We had been years-long patients elsewhere, and had experienced four failed IUIs and two rounds of IVF yielding only one embryo and subsequent miscarriage. We were tired, sad, and wondering if becoming parents was achievable. Our previous doctor told us we would be “lucky” to end up with one child, and suggested egg donation. After researching different fertility specialists online and comparing SART statistics, I knew Dr. Miller would be the best choice for us.
When we met with Dr. Miller, he had a thorough knowledge of our history, a plan, and compassion for what we had been through. I have PCOS and thyroid disease and felt that my previous clinic did not take this into account when creating my treatment plan.
Dr. Miller took my concerns seriously and addressed them. I had concerns about insulin resistance, he investigated it and treated it. I had concerns that my previous clinic did not take my thyroid disease seriously enough and allow for appropriate monitoring, he agreed and made sure my levels were optimal before proceeding. My husband was concerned about his inconsistent fertility testing, Dr. Miller confirmed that we were dealing with an element of male factor infertility.
After our first meeting, I distinctly remember him saying, “I might not get it the first time around, but I’m confident we will get you on the right treatment plan.” Well, he did get it the first time around. Imagine our surprise and delight when on our first round with Dr. Miller we ended up with five beautiful embryos, and a pregnancy on our first transfer. He and his staff celebrated with me each week when things were going well in my early pregnancy, and by the time I “graduated” these people felt like family.
Today, we have a beautiful baby. When recovering in the hospital, my husband asked me if I thought Dr. Miller knew how much he changed our lives. When we had no hope left, he gave us everything. I think about this time last year, and not in my wildest dreams did I think I would be where I am today. I spent six years of Christmases thinking “Next year will be my year.” Now, I look at my daughter and have to pinch myself. I can’t believe she’s here!
My advice to those going through this is to live while you’re waiting. It’s tempting to throw everything you have into the process when you’re going through it. One month off from treatment to take a vacation or celebrate something special is good for your mind and body- don’t forget to nurture yourself.
Patient Story- Sheri

“We have been very blessed with great kids who seem to appreciate life, maybe because somehow, subconsciously they know that it took that extra little miracle to be here.”
Up until now, our patient stories have featured women who have recently become mothers. However, today’s submission is from Sheri, who first became a patient 20 years ago! Technology has advanced over the years, but the overarching message from Dr. Miller remains the same: “trust the process.”
My story begins many years ago (my two miracle babies are now 19 and 16)!
After years of trying to conceive, being on countless fertility drugs, endless testing and 5 years of monthly disappointing moments we decided it was time to take the next infertility step and meet Dr. Miller. My husband and I immediately felt confident he was the answer to our unexplained infertility. We left with a sense of relief. He looked us right in the eye and said “trust the process.” It was Dr. Miller’s confidence and stellar reputation that made us say “When can we start!”
The process, although long and hard at times was, by far, made less grueling and easier to face because of Dr. Miller and his staff. Every single person we encountered was kind, sympathetic, positive, caring and made us feel like they were our “infertility family”. There was one person in particular who will always stand out and be a part of my heart and that was Lynne who was at the front desk. Her smile when I walked in put me at ease instantly.
Infertility is praying endlessly. It’s sad, depressing, hard, lonely and you shed many tears. There are many roadblocks and setbacks but this journey with Dr. Miller was worth every single minute.
We were very fortunate that our first round of IVF gave us our son and our second round gave us our daughter.
Both of those IVF cycles began as multiple pregnancies but by some miracle our son and our daughter held on when we experienced vanishing embryos. It was terrifying to think we were losing the babies. I remember the moment when we thought we were miscarrying. Dr. Miller was in Europe and he called personally to ease our fears and tell me what to do to give the other baby the best chance. Grief hit hard knowing our multiples were now single pregnancies. I still think of what would have been had that not happened but take a moment to remember them and even though we never met them we love them always for what little time they were ours.
A year after our daughter was born we kept trying for more children without success. Time was not on my side because of my age. Dr. Miller saw me struggling mentally and finally gave me the strength to walk away and enjoy the 2 miracles we were blessed with.
Our son, Nick, is now 19 and studying engineering at Purdue and our daughter, Emily, is 16 and thriving in high school. Every moment of their lives has been better than the next. We have been very blessed with great kids who seem to appreciate life, maybe because somehow, subconsciously they know that it took that extra little miracle to be here.
To all the patients present and future…I pray for you, I wish you peace always and I hope your dreams come true. You deserve to be parents!
Patient Story- Breda

“Not everyone will understand IVF or be able to relate, so it’s important to surround yourself with support. More people than you realize struggle with infertility.”
Today’s patient story is from Breda. After not finding success or feeling comfortable at another fertility clinic, Breda came to us. We are all glad she did! Dr. Miller was able to diagnose her with endometriosis and after surgery and IVF, she was able to get pregnant. Breda is due in January!
Breda writes:
I met my husband later in life and we got married when I was 38. I was and still am wary of the stigma of older mothers, even though being older is accepted. I’ve always wanted a family and we started trying right away, but I had three miscarriages in a year and a half. I was at a different fertility clinic for a year, but didn’t feel comfortable there. My husband’s colleague recommended we see Dr. Miller and what a difference!
We first met online during COVID and Dr. Miller told us, “You’ll be a mother, kiddo.” He was so kind, didn’t rush us, and he explained everything. He learned I was an English teacher and told me a story that put me at ease. He never stopped his storytelling, and I welcomed his personable demeanor after some bad experiences at the previous clinic. Dr. Miller found issues that the previous doctor did not, including endometriosis.
After a biopsy, Dr. Miller found abnormalities in my uterus and I was diagnosed with Level 1 endometriosis. During surgery, he removed five spots on my uterus. I also had the Endometrial Receptivity Assay biopsy to determine the receptivity of the uterus to implantation. Soon after, we had an egg retrieval and two transfers.
Throughout this process, Dr. Miller and his staff explained everything so thoroughly and never seemed irritated or disinterested when I had questions. I also got to know Dr. Miller and the nurses because they talked to me during appointments. I always felt people cared and were invested in our success. I felt so secure going into our procedures and never felt anxiety or stress visiting the office.
Even though our first transfer failed, a second embryo implanted and I will never forget that experience. Dr. Miller, Courtney, and Melody were present for the transfer, and made me feel so comfortable. Dr. Miller even told us a funny story about meeting an actor from Will & Grace. While we waited after the transfer, my husband and I held hands and prayed, and we also talked about how wonderful it would be if it worked. Many times, we dreamed of finishing our nursery and being able to move forward with our plan. The transfer worked, and our baby is due January 8, 3.5 years after we began IVF and what seems like a million doctor appointments.
I was very nervous the first 12 weeks of my pregnancy and braced myself for bad news, but at every ultrasound Courtney reassured me with her positivity. We are so grateful for everyone at the Naperville office.
It took until I was about 20 weeks pregnant for me to relax and realize we’re finally going to be parents! I’ve cried many happy tears for a change! Not everyone will understand IVF or be able to relate, so it’s important to surround yourself with support. More people than you realize struggle with infertility. Meditation and journaling are helpful (as well as long walks with our dog, my first baby). Finally, never stop hoping and praying, even if you’re an older mother!
Patient Story- Julia

“This is why you keep fighting; so that you can have peace. Whatever outcome will bring you peace, that is what you fight for.”
Julia is a patient that our office has known for quite some time. She recently welcomed her third baby boy and we have enjoyed getting updates and pictures throughout the years. A seasoned IVF veteran, Julia has been through it all and yet she is incredibly candid about her experience. This openness has led her to volunteer to answer calls for the Resolve support line twice a month. While there aren’t many calls, she is so grateful when she gets to speak to someone and give them some hope. We are so grateful that Julia has shared her story.
She writes:
The other day, I took my two older boys to the fire station open house. It was absolutely packed, it seemed like everyone from our town was there. I looked around at all of the children, moms, dads, siblings, grandparents, etc. and had a moment of self-doubt.
“I don’t belong here,” I thought to myself. “This event is for families.”
As if on cue, my middle son reached up to hold my hand, and my older son ran ahead and called out for me. “MOM! This way, follow me!”
I was instantly brought back to reality, my feelings of insecurity disappearing and belonging restored. I am a mom (of three boys!), and I DO belong at family events, school drop-off, parent-tot classes, parks and baby pools, and in the club that is Parenthood.
The lingering grief and pain of infertility can rear its ugly head at the strangest moments, like it did that Saturday morning. I remember the feeling of fear so well; the fear that I would never become a mom. I know all too well how painful the treatments and the unknowns are as I fought long and hard for my boys. However, I also know the peace that comes from a dream achieved. I want to instill hope in anyone who has that fear and pain, who is in the throes of fertility treatment, who is struggling with self-doubt and the unknown.
I have three beautiful and healthy boys. They are almost perfectly spaced apart; 2.5 years. From the outside looking in, we are a very typical family. And in most senses, that is correct – except for how our family was created.
We waited four years for our first son. I worked for one year with my ob-gyn and Clomid. I then had six stimulated rounds with my first fertility specialist and one miscarriage. When I met Dr. Miller, I had two more failed IVF rounds before we chose to use a donor egg. I had a polyp removal surgery. I did three trial cycles to determine the optimal window for an embryo transfer. We lost our first donor due to poor response to stimulation while I was on hormones alongside her. With our second donor, my first transfer was a blighted ovum that ended in two separate D&C surgeries. After extensive blood work, I was diagnosed with MTHFR, a genetic blood-clotting disorder that can affect implantation.
On November 9, 2016, my 13th cycle, I became pregnant with my first son.
Charlie was cycle 13. James was cycle 15. John was cycle 16.
I share the details of my journey not to overwhelm you, but to give you strength. Maybe your journey will be shorter than mine. Maybe it will be longer. It often felt daunting, hopeless at times, and never-ending. I remember the receptionist at Dr. Miller’s office pulled out my file. It looked like several copies of the Yellow Pages stacked on top of each other. During one of my meetings with Dr. Miller, he put his hand on top of that file and said, “Julia. We haven’t been through this much, for you to not get pregnant. I WILL get you pregnant.” I trusted him and pushed forward despite the fear and pain.
This is why you keep fighting; so that you can have peace. Whatever outcome will bring you peace, that is what you fight for. And you will know when that time comes. People ask me how I did it. They want to know how I managed the appointments and driving, the shots and tests, the physical side effects and emotional trauma, the disappointment and the grief.
I tell them the truth; you just do it. You have to keep going so that you can have your peace.
I promise that the grief and fear will fade with time. It might make an appearance here and there after you have achieved your dream, but that is just a little bit of PTSD from the journey. It will fade. You will hold your little miracle, you will walk with your child at the fire station open house, or into that parent-tot gym class, or to the first day of preschool, or story hour at the library and you will belong. You will feel peace.
Believe in Dr. Miller. Believe in his nurses, the ultrasound techs, the phlebotomist, his entire staff. Throw in some prayers, push forward, and wait for your time to come.
Patient Story- Rachael
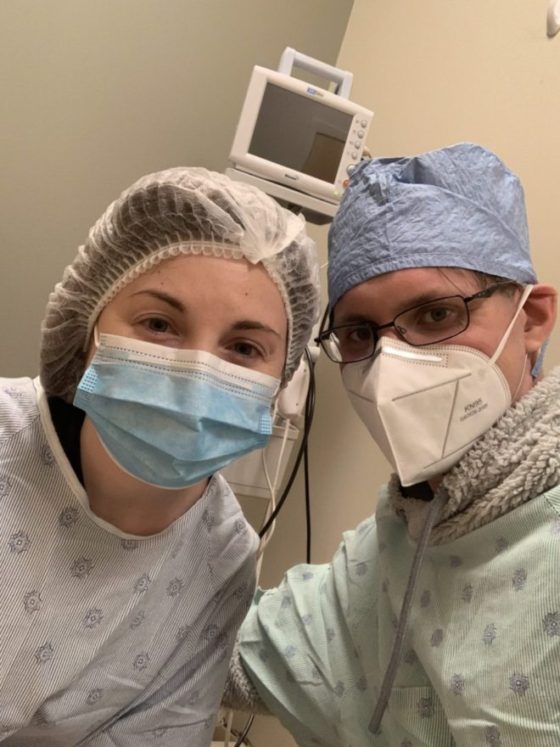
“Our plan was always to have a baby, but our path certainly wasn’t a straight line.”
Our next patient story is from Rachael. Rachael’s journey to motherhood has not been an easy one. After undergoing several unsuccessful rounds of IVF, Dr. Miller advised Rachel to consider using an egg donor. In her story, Rachel describes the process she and her husband went through to choose an egg donor and what advice they would give to others in her situation. Rachael’s story has a happy ending- she is now pregnant and due with a baby boy in February!
Rachael writes:
To say that our journey was a difficult one is an understatement.
I was 34 years old when we wanted to start our family. After six months of trying on our own, we met with Dr. Miller. Testing and medication followed, and we eventually discovered – after finding out I had a diminished ovarian reserve, as well as confirming that I had a unicornuate uterus – that IVF was a route we needed to take. We diligently went to work ordering medication, setting up appointments, and saying so many prayers. Unfortunately, our first round failed. We just kept thinking, “This is it!” only to find ourselves back at square one.
When I met with Dr. Miller for our follow-up consult, he had another plan to try again. Upon leaving our meeting, he told me, “Stick with me, Rach! Rome wasn’t built in a day.” Knowing this was true, and knowing we had faith in our doctor, we trudged ahead and kept going. What followed were an additional five rounds (some stopped before retrieval), further testing and added medication, laparoscopic surgery, and the need to put on more weight in hopes that it would help my egg quality.
After several additional rounds of IVF and additional embryos from said rounds that didn’t take, our insurance plan was running out of options for us to keep moving forward. Dr. Miller advised us not to do the egg retrieval with my own eggs at that point and suggested turning to an egg donor. We were absolutely heartbroken. We knew that this was a real possibility, but the news was hard to take in. We were at the end of stimulation injections, and my body just wasn’t cooperating (which had happened during another of our previous cycles). Knowing my track record, Dr. Miller was concerned that this round would not work and then we’d really be out of options with my insurance. We converted the round to an IUI, but it didn’t take. A month later we transferred the one frozen embryo we had (insurance would still cover that), but we were left with a negative result.
We were angry, frustrated, and beyond depressed. We knew it was no one’s fault (I had to keep reminding myself that I did nothing wrong), but we couldn’t understand why it was happening. We did absolutely everything we possibly could to have a positive outcome, but were left with nothing but grief. You know everyone means well when they offer their condolences, but there are times when IVF is an incredibly isolating experience.
A few months later, we met with Dr. Miller again to discuss using an egg donor. He answered all our questions and felt optimistic about this new plan. When we were ready, we contacted an agency to get information. Later that fall, we chose our egg donor and started to feel more optimistic ourselves. Our donor went through the testing process and started some medication. We had psychological evaluations to make sure that everyone was in the right state of mind to go through this process, and we met with a lawyer to go through the contingencies of everything.
Our donor finally had her egg retrieval in February; we received 48 eggs (which was incredible!), and out of the 48, we had 17 embryos to freeze. We couldn’t quite sync up cycles, so we worked toward an April transfer, but then that got canceled due to me catching COVID-19. We were finally able to complete our transfer in May, and at the end of the month we received our first positive pregnancy test! I’m due in early February with a boy and am currently 18 weeks along (for a frame of reference, I am now 39 years old).
Moving forward, we have 16 embryos at our disposal. Besides some days where I didn’t feel great in the first trimester, my energy has bounced back in the second trimester and I feel pretty good! We’re really looking forward to the future and still cannot believe that we’re on the other side after years of wondering “what if?”
It was a long, difficult four-and-a-half years to get to this point. There were so many tears, early morning appointments, and hours upon hours of frustrating phone calls with insurance and pharmaceutical companies. There were so many pregnancy announcements by friends and family. There were so many times when we felt raw, numb, and alone. But on the other hand, we had hope. We had a strong support system, and we had a caring doctor who genuinely wanted the best for us. Dr. Miller’s staff was so kind and offered me hugs on more than one occasion when we received bad news. We learned to give into the unknown (something difficult for us teachers to do) and trust that we were doing everything we could.
If I can offer advice, I’d stress the importance of learning to pivot. Our plan was always to have a baby, but our path certainly wasn’t a straight line. We had to adjust the details of our dream, but that doesn’t mean that we’ll be any less of parents than we would have if things had worked with my genetics. Our dream could still be a reality, but adjustments were needed. Keep the end goal in mind: if it’s to have a child, understand that what that means might look different than what you anticipated when you started the journey.
If you find yourself in need of an egg donor (or sperm donor, if that’s the issue), I’d encourage you to take your time and go through the process when you’re ready. Don’t try to look for yourself in the pool of applicants; you won’t be there, and that’s okay. When we first got information from the egg donor agency, they encouraged us to not pay as much attention to pictures, but to focus on the information: we examined their health history and that of their relatives; we listened to their reasons for being a donor; we screened applications for the possibility of twins and triplets (given my unicornuate uterus, multiple births at one time was not considered a viable option); we also poured over their previous donor cycles to see what kind of success they had.
In the end, we chose someone who looked happy. She genuinely wanted to help other people conceive and assisted others in that goal already. The agency (and Dr. Miller’s office) couldn’t say enough good things about her, which was really reassuring. Besides matching my ethnicity, she does not look like me, but I’m keeping in mind that our boy very well may look more like my husband than the donor. If he doesn’t, that’s okay, too. This was something I had to learn to get comfortable with before we officially went through the donation process.
There are times when I look back at the last few years and the pain comes crashing back, and I’d be lying if I said it was easy to move on from my genetics. However, at the end of the day, the goal is to have a baby, and I learned that it is still possible if my genetics are no longer an option. This could be a path for you, too.
We would also encourage you to let people in and have a support network. My husband and I did not always want to talk about our struggles, but knowing we could speak with family and friends was helpful (and there are other support groups if you aren’t getting the support you need from those around you, too). Even though most of the people you know might not “get” the struggle you’re going through, it’s important to remember how many people are in your corner. You’re going to feel alone. You’re not.
Keep the faith. We’re rooting for you!
Patient Story- Courtney

“Keep going even when it feels like you can’t… The little victories will give you strength.”
Today’s patient story is from Courtney. Courtney discovered she had endometriosis when she and her husband were not able to conceive naturally after several months of trying. After undergoing surgery with Dr. Miller, she was able to get pregnant via IVF and just welcomed a baby boy only three weeks ago! Congratulations Courtney!
Courtney writes:
My husband and I began trying to conceive in late 2017. While at my yearly gyno appointment in May 2018, I mentioned we were trying to conceive. I was told to track ovulation with an app and/or pee sticks and go from there. My period had always been like clockwork and I learned that my ovulation was too. I maybe had heavier/more painful periods but nothing that ibuprofen and a heating pad couldn’t fix. My gynecologist did an internal ultrasound and noticed that one ovary was dense, leading her to believe that I might not ovulate on that side, however my pee sticks indicated that I did.
We ended up getting pregnant on our own in the summer of 2019, but that ended in a miscarriage (D&C) as there was nothing in the sac. I then had the dye test to see if my tubes were blocked and they were not. I also did 3 rounds of clomid with no pregnancy. This was the end of the road with my regular gynecologist as she couldn’t help me any further.
I then went to another gynecologist in my hometown to move onto IUIs. He did a natural IUI with no luck. Then we tried a medicated (clomid) IUI with no luck either. During this process, he did an internal ultrasound and that’s when I first learned I possibly had endometriosis. He referred me to Dr Miller.
I had laparoscopic surgery with Dr. Miller in Feb 2021 for endometriosis. We decided to try surgery before an egg retrieval, because Dr. Miller thought he could clean me out and then we could try to conceive naturally or with clomid as he didn’t think the endometriosis was as bad as it turned out to be. However, during surgery he found stage 4 endometriosis on my ovaries and appendix. He removed my appendix and did what he could on my ovaries in order to preserve them for IVF.
After my surgery, Dr Miller said that the endometriosis had been there for quite awhile because the cysts were so fixed to my ovaries. He said he did what he could to minimize the cysts but he couldn’t get rid of them fully because that would ruin good ovarian tissue for IVF. After I’m done having kids, I can have another surgery to fully clean me out.
It was invaluable to have Dr. Miller as my surgeon and fertility specialist. The entire time he was focused on the goal at hand- to have kids. I felt comfortable during the process that he knew what to do during surgery to make it possible for me to have kids.
After surgery, we started preparing for IVF and I had my egg retrieval in July 2021. We ended up with 4 well graded, untested embryos after retrieval. My first FET (frozen embryo transfer) was in September 2021 and unfortunately ended in a chemical pregnancy. Shortly thereafter, we did another transfer and I gave birth to my son, Leo, on August 11.
Going through infertility takes a toll on you emotionally and physically. Here are a few pieces of advice I would give to other women dealing with infertility.
- Keep going even when it feels like you can’t do/go anymore. The little victories will give you strength. For example, the recovery from retrieval was brutal for me, but when we found out we got 4 embryos, I felt like I could do it all over again.
- Ask for help and allow help from others. I am the most organized person out there but I had to have my husband take the reins on the meds because it was all too much for me. I never prepared, mixed, set up, or gave myself one shot!
- Don’t change your lifestyle. Dr Miller never once told me what to eat, drink, do, or not do. Working out was limited with retrieval and FET, but that was the extent of it.
- Take the month off and go on vacation. Dr Miller wrote in my message on the portal that this was a must! You have to continue to live your life as best as possible!
COVID-19 Vaccine and Pregnancy/ Breastfeeding
Fertility History: Learning About Your Mom’s Fertility Journey to Help with Your Own
With a baby, who’s the first person you’ll usually call for help? If you’re lucky, your mom is usually only a phone call away to dispense parenting advice and tips for soothing a fussy baby.
But even before that, it’s a good idea to seek out her perspective on having children and the fertility journey she took to get there. When considering your own fertility history, you may want to consider digging into your family's medical past. The process of becoming pregnant can be a daunting task. And just as it helps to have a lot of support when the baby is born, you may want to have her help offer some insights into what you might face when it comes to pregnancy. Of course, you don’t have to tell her that you’re starting your own journey tomorrow or next week or even next month, but think of it as a perfect and valuable bonding opportunity between you and Mom.
You might be thinking, we aren’t the same person! How does her fertility history compare with yours? Well, for one, you can ask her about any medical conditions or fertility problems she faced when she was trying to get pregnant or during her pregnancy. It helps to gather some family history that the doctor may ask about, particularly if you may exhibit some similar traits. At the same time, while some conditions are genetically passed down, you should also be aware many other factors came into play during her pregnancies. Her age, health, environment, stress levels, diet, and your father’s health and lifestyle habits would all influence fertility and pregnancies. Not only that, modern medicine has changed so rapidly since you were born, so what might have been an issue for her back then may be handled or treated very different today.
However, talking to your mother, or even both your parents, can help give you more information than you realized you might need about your fertility history. Not only will you learn more about family medical history, but you’ll learn what it was like for them – the anticipation, the nervousness, the frustration, the questions they had for their doctor at the time. They may reveal some funny stories that you didn’t know before that might help you get excited about creating your own stories with your partner. You may realize that any fertility history questions or fears you had about family planning were not that different from what they went through to give birth to you.
Some fertility history questions you can start the conversation with:
- How long did it take for you to become pregnant?
- How old were you when you first decided to try?
- Did you have any issues?
- Did you have irregular menstrual cycles?
- Was there any family history of infertility?
- What about endometriosis, fibroids, or PCOS?
- Did you or any siblings ever have a miscarriage?
- Did you or anyone go into premature labor?
It’s also helpful to talk to any siblings, aunts, cousins, or even good friends about their individual journeys with pregnancy and their fertility history. Beyond the medical component, people often want to share their experiences, both good and challenging ones, and can help provide much needed support as you move through your own journey. Most importantly, you’ll realize that you’re not alone, and while everyone’s fertility story is their own, it’s a story that connects women on a profound and extremely special level.
Avoiding a Second Surgery: How a Change in Medication Could Lead to Pregnancy
Our last blog post detailed a successful isthmocele repair surgery that will hopefully lead to a healthy pregnancy. Today’s post is a little different.
Here is a case where surgery, performed by another surgeon, had failed. The patient, Lindsey*, was still symptomatic with fluid in the cavity. Dr. Miller provided the patient with a new medical protocol, avoiding a second surgery.
Read Lindsey’s story to find out the result.
After almost four years of struggling with secondary infertility, I was fortunate enough to discover Dr. Charles Miller and the Advanced IVF Institute. I had been diagnosed with an isthmocele, which was a defect in my cesarean scar that was leading to fluid accumulation in my endometrial cavity. Just reaching the diagnosis of an isthmocele and the potential impact it could have on my fertility had taken many years. I was exhausted, frustrated, and unsure if I would ever have another child. My local physicians seemed to be at an impasse. Despite having my isthmocele surgically repaired, I was continuing to develop fluid which was impairing the ability of my physicians to transfer any embryos.
After contacting Dr. Miller, I knew it was the right decision. He was very resolute in the forward management of my situation. He did not recommend a repeat surgery to repair the defect that had not been successfully repaired. This was initially surprising to me! Repeat surgery seemed to be the obvious decision, but his thoughts were that possibly changing the protocol for my Frozen Embryo Transfer (FET) would decrease the amount of fluid I was producing.
When transferring frozen embryos, the usual protocol is to use estrogen and the route can vary (i.e. oral, patch, intramuscular). The patient then adds progesterone prior to the transfer. Unfortunately, in my case, the estrogen caused a build-up of fluid, particularly with the isthmocele.
Due to his extensive experience in this matter, I trusted Dr. Miller’s judgment and I am so thankful that I did. After two previously canceled FET cycles with other protocols, I followed the protocol set forth by Dr. Miller on my third attempt.
The protocol that he recommended, and he said was successful on many occasions, is that rather than utilizing estrogen initially, the meds are used to stimulate the ovaries so that my own estrogen levels rise. Thus, taking away the need to utilize estrogen.
I am ecstatic to say that it worked and I am eternally grateful to Dr. Miller and his staff. We are set to welcome our miracle in May 2018!!
-Lindsey
*Name changed to protect patient privacy
Recognizing Gynecologic Cancer Awareness Month: The Importance of Hereditary Cancer Screening
Did you know September is Gynecologic Cancer Awareness Month? The five main gynecologic cancers consist of ovarian, uterine/endometrial, cervical, vaginal and vulvar. According to the Foundation for Women’s Cancer, more than 109,000 women will be diagnosed with a gynecologic cancer this year. That’s why it’s important to screen our patients regularly or recommend genetic testing if family history does in fact point to these gynecologic cancers.
Female gynecologic cancers can be sporadic, meaning, it doesn’t have to run in the family for the cancers to appear. You may not love your annual pap smear, but the quick, non-invasive test allows us to screen for cervical cancer and signs of pre-surgical changes. You also may dread the day of your screening mammogram, but it can help us detect changes to your breasts that cannot be felt with an exam, as well as early changes that are otherwise undetectable. If cancer is identified, our goal is to find it in its earliest stages to have better chances of eliminating it. As such, these screenings, although sometimes uncomfortable for you, can be lifesaving.
Despite the fact most cancers are not inherited, there are some family histories that are concerning for inherited forms of cancer. For example, when you visit your doctor, you are asked about your personal and family history for high blood pressure, stroke, diabetes and heart disease AND we also ask about any cancers in your parents, grandparents, aunts, uncles, siblings and children. If your family history does point to gynecologic cancers, we may recommend early and more frequent screening than the general population or determine you are a candidate for genetic testing.
Genetic testing evaluates your DNA (genetic material), and identifies whether you may have a genetic mutation (change in your DNA) that places you at an increased risk for developing different types of cancer, depending upon which mutation you have. Some mutations include the BRCA mutation that places women at increased risk for breast or ovarian cancer or Lynch syndrome that places one at increased risk for ovarian, uterine and colon cancer. It does not test your cells to see if you currently have cancer or will develop cancer, but instead gives you information on whether you have an increased risk of cancer compared to the general population.
Genetic testing involves counseling about what information the test can provide, the recommendations based on the test results, and the limitations of the test. If you and your physician decide that you are a candidate for testing, your blood is drawn and your results will return in 2-3 weeks. If you test negative it does not mean that you will never develop cancer, but rather you do not have a known inherited mutation that places you at increased risk for developing certain types of cancer. Conversely, if you test positive it also does not mean that you are definitely going to develop cancer, rather you have an elevated risk of developing certain types of cancer (range of 4%-80% risk depending upon the gene and type of cancer). For those that test positive, counseling can be provided and next steps will be discussed.
At the Advanced Gynecologic Surgery Institute, we are dedicated to you as your health advocate. We are here to offer you the best possible support and expertise through our many years of experience. If you want more information regarding hereditary cancer screening and testing, please contact our office: https://drcharlesmiller.com/request-a-consultation/.
To your continued health,
-Dr. Kirsten Sasaki




