Her Own View: A Patient’s Journey Through IVF (Day 12-25) Adventures in Egg Retrieval
Hi everyone!
I’ve had loads of activity since the last time I updated! Since my last post, I had a third and fourth ultrasound, an egg retrieval and had my embryos shipped to the lab for genetic testing! Yes, a lot can happen in just a few days! Let me break it down…
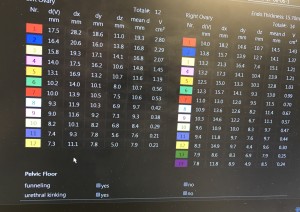
During my third ultrasound, they saw 12 follicles in my left ovary and 14 follicles in my right ovary. I’ve included a picture so you can see they were still small that day. The size is in the “mean d mm” column. For a follicle to be considered mature, they must be between 16-22mm.
Dr. Miller requested I come back the next day after he increased my Menopur and Follistim to see if I was ready to pull the Human Chorionic Gonadotropin (HCG) trigger. The HCG trigger shot gives your follicles one last push before the egg retrieval. The shot happens exactly 35 hours before the retrieval. The next day, I had an ultrasound, and I was ready to pull the trigger at exactly 8:30 PM because I was scheduled for my egg retrieval 35 hours later at 7:30 AM. The shots during this time period were not too bad, but by the end, I was very bloated, which is a normal side effect of the medications. Yoga pants, loose tops and layers were my wardrobe staples!
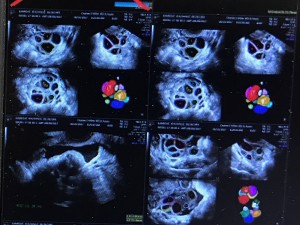
So here we are, the day of the retrieval! I had to be at the office at 7 AM, for my 7:30 AM egg retrieval procedure. The staff took me in at exactly 7 AM, where they had me change into a hospital gown and gave me discharge instructions. The Anesthetist then hooked up what she needed to, and told me what to expect. The Embryologist also came in and went over the plan (egg retrieval/ freezing embryos, and Preimplantation Genetic Screening (PGS). She mentioned that there would be one update the next day, and we would not get another update until 5 days after that. The staff then took me into the procedure room where I was injected with the anesthesia. The next thing I knew, I was up and with Dan! I think the actual procedure only took 15 minutes. The first thing I heard was, “they got 30 eggs!” The staff was extremely attentive during recovery (about an hour) and Dr. Miller paid me a visit and said he was very pleased with the retrieval. After the procedure, I took it very easy and napped the rest of the day. I did take a drive with Dan that night to run an errand, which did not go well. I threw up when I got home, probably from the anesthesia and motion sickness from the car! And that is why it’s important to have a driver the day of the retrieval! The procedure was on a Sunday, and I managed to go to work on Monday, although I had to leave early. I felt uncomfortable for the next few days, but that is a normal side effect.
The next day, I received a call saying, out of the 30 eggs, 26 were mature, and 22 fertilized with ICSI (Intracytoplasmic Sperm Injection). Since I had so many eggs, Dr. Miller put me on a few medications to minimize the risk of Ovarian Hyperstimulation Syndrome (OHSS).
Often times once the retrieval takes place a transfer can be done on Day 3 or Day 5 after the embryos have matured under the care of the embryologist. This is called a fresh cycle because the embryos are “fresh out of the oven.”
However, because we chose to do the PGS testing our transfer turnaround time is a little longer. On Day 5, the lab was happy to report that I had 10 normally developed embryos that could go on to be tested for genetic normalcy. Those results should be back any day and we will then know how many viable embryos we have. After that, we will also be going through a frozen cycle. This means the embryo(s) will be thawed and then placed into their new home (aka my uterus).
To be honest, I’m enjoying this time where everything is basically out of my control. Let’s see what happens. Stay tuned!
-Katie
Her Own View: A Patient's Journey Through IVF (Days 4-11) Shots, Shots and More Shots
I have a few things to update. I started ovarian stimulation and had my first two monitoring appointments. The first appointment was 6 days ago and they took an ultrasound of the uterus to see what’s going on in there. They saw about 18 follicles on that first ultrasound, so they decided to start me on the Menopur (two vials), Follistim (150 units), Lovenox (one pre-filled injection) in addition to the Lupron. Yes, my friends, that’s four shots that I’m injecting into my belly every day! Some women want their husbands to do it, but I decided I wanted to do it myself. I think the mental aspect of taking four shots a day is a lot, and if you must coordinate with your husband to do these shots two times a day, it really adds another layer of complication--so, I stick myself! It’s kind of empowering, believe it or not!
Ok, the shots are NOT BAD! For the Menopur, I have to mix two vials of powder and one ML of solution. There are loads of tutorials on how to do this, so it’s not hard at all. This one does burn a little, but again, not too bad! Follistim is a pen, no mixing with this one. Burns a little, but again, it’s not bad. The Lovenox is by far the worst one. It burns going in. The first time I injected this one, it was PAINFUL! But, since that first injection, my expectations were set and I knew it was going to hurt. And now I’m used to it. If you make it this huge deal, then yes, it will be a huge deal. If you think of it as just part of your day, it’s no big deal. Wash your face, brush your teeth, give yourself your shot….done and done! Move on to the next thing! Also, I’ve not really felt any side effects. I’m bloated, but that could have just been the brownie I ate last night!
On the second ultrasound, they saw over 20 follicles, but all under 10mm. That means they are all small, and they need to keep stimulating me. After the appointment, they increased my Follistim to 300 units from the 150 I was originally on.
Dan and I also had to start an antibiotic to reduce the risk of infection at the time of retrieval. My next appointment is tomorrow, so I will update next week!
Thanks so much for reading!
-Katie
*Please note that each patient’s case is unique and Dr. Miller creates individual care plans for each couple based on their medical history.
Her Own View: A Patient's Journey Through IVF (Day 1-3)
Today we’re excited to share with you a new blog series about Katie, a patient of Dr. Miller’s, who has experienced difficulty conceiving. She will be sharing her fertility journey with us in her own words. Katie’s goal for journaling her journey, is that you might find comfort and strength in hearing from someone who is also going through the process as well, whether you are going through it now, or are pregnant after months (or years) of trying. Her struggle may be different, but her hopes and dreams of reaching the end goal, that bundle of joy, are the same. Although the outcome is unknown, Dr. Miller and his staff are excited to work together with Katie and her husband, Dan, as their partner and guide.
Hello Everyone!
My name is Katie and I would like to welcome you to my very first patient blog post! I’m excited to take this fertility journey with you. To give you some background, my husband, Dan and I are 31. After getting married in 2011, both Dan and I went to graduate school, which wasn’t the ideal time to start a family. Finally, at the end of 2015, we were ready to start our family. We officially started trying to conceive (TTC) in December 2015. To our surprise, we got pregnant the very first month of trying! Unfortunately, in March 2016, we lost the baby at twelve and a half weeks, a few short days after we told close family and friends. Since I had the miscarriage at home, we were not able to test for genetic abnormalities. My OB said over 50% of miscarriages happen because of genetic abnormalities, so that was most likely the reason. The entire experience was truly heartbreaking!
We were told by my OB to wait one cycle before TTC again. Since I had a D&C*, I didn’t get my first period until May 2016. In July 2016, we were pregnant again, which resulted in a chemical pregnancy* at 4.5 weeks. My OB decided to do a Recurrent Pregnancy Loss (RPL)* testing. Those tests indicated that I might have a blood clotting disorder; however, those tests were inconclusive.
My OB suggested we try again since my tests didn’t indicate any real red flags, but to take baby Aspirin for the possible blood clotting issue to be on the safe side. So we did try again, and we were pregnant again in October 2016, which resulted in another chemical pregnancy at 5 weeks. At that time, my OB agreed we should see a Reproductive Endocrinologist (RE).
After performing extensive online research, Dan and I decided to schedule a consultation with Dr. Miller in November 2016. I chose to see Dr. Miller because of his excellent reputation and success rates. Before he came in to see Dan and me, Dr. Miller reviewed my case. He said since I have an unknown reason for my recurrent losses, he would like everything tested-- from semen to genetics to blood. You name it, he’s testing it! Since I’m an HMOI patient, and Dr. Miller uses a lab outside the network, the tests had to be done through my OB.
The tests indicated that I have a MTHFR gene mutation*. This mutation does not allow synthetic folic acid to be absorbed into my body, so Dr. Miller gave me a prescription that would allow my body to absorb folic acid. I was hopeful that maybe this could be the answer.
During this time, Dr. Miller also had us do a Clomid* 50mg test cycle to see how my body would respond, but let us know that we would not be TTC just yet. We found that my progesterone was 15 Mg/Ml, lower than the 20 he likes to see with a medicated cycle. Perhaps this was another clue?
In early May 2017, we had our follow up appointment with Dr. Miller, and he talked us through all our options. He said the reasons for my recurrent losses are most likely due to a blood clotting issue or genetic abnormalities. He said we had three options:
- Clomid 100mg with Lovenox*
- IVF/ICSI* with Lovenox (50% live birth rate/ 16% chance of loss)
- IVF/ICSI with Lovenox and Preimplantation Genetic Screening (PGS)*. (70% live birth rate/ less than 5% chance of loss)
We decided to go for option 3! IVF with PGS!
So, here we are! We will do the egg retrieval in June and transfer in July! I’m currently on Lupron * 10 units, which I’ve been taking since May 23rd. Surprisingly, this injection is not bad at all. The needle is tiny and it’s relatively pain-free. I just got my period (finally!), making my cycle 32 days (very long for me as my average in 27 days). I’ll be starting my stimulation shortly here after an ultrasound in the coming days! The plan is to continue the Lupron and add Menopur* and Follistim*. The IVF nurses are really good at keeping me informed on next steps, and I also have a clear written protocol from the office.
I am cautiously excited about the next two months, but I’m not trying to get ahead of myself. I think the most important thing is to take it one step at a time, and not get too into my head about the whole process!
I’ll be updating on my IVF journey a frequently as I have new things to report!
-Katie
Katie's TCC Timeline
- 2011 – Married! Excited about life together!
- December 2015 – Removed the goalie! Let’s try to have a baby!
- March 2016 – 1st miscarriage at twelve and a half weeks. Heartbreaking. Maybe just an unfortunate fluke? Genetic abnormalities? Unknown. D&C to follow.
- July 2016 – Pregnant again! Chemical pregnancy 4.5 weeks. What’s going on here?
- August through September 2016 – Recurrent Pregnancy Loss (RPL) testing. Maybe a blood clotting issue?
- October 2016 – Pregnant again, and you guessed it…another loss at 5 weeks.
- November 2016 – Started seeing Dr. Miller. Discovered MTHFR gene mutation.
- March 2017 – Test Clomid cycle. Low progesterone.
- May 2017 – Starting IVF/ICSI with Lovenox and Preimplantation Genetic Screening (PGS). Taking Lupron 10 units since 5/23/17
- June 2017 – Got my period, waiting to go in for a baseline ultrasound and starting simulation for the retrieval!
Glossary
D&C: also known as dilation and curettage, a surgical procedure in which the cervix is opened (dilated) and a thin instrument is inserted into the uterus. This instrument is used to remove tissue from the inside of the uterus (curettage). ACOG
Chemical Pregnancy: occurs when the pregnancy hormone is elevated (i.e. beta hCG), but there are no other signs of pregnancy and it is too early to be detected via ultrasound (ivf.drcharlesmiller.com)
Recurrent Pregnancy Loss (RPL) Testing: examines genetics, infection, autoimmune testing, thrombophilia (blood clotting issues), the structure of the uterus and hormonal concerns (ivf.drcharlesmiller.com)
Clomid: Clomiphene stimulates the release of hormones needed to cause ovulation. Clomiphene therapy is typically used for 5 consecutive days early in the menstrual cycle, for 3 to 6 monthly cycles. It may take several cycles to find the right dose to stimulate ovulation. After that dose is determined, a woman will take the drug for at least 3 more cycles. If she does not become pregnant after 6 cycles, it is unlikely that further clomiphene treatment will be successful (ivf.drcharlesmiller.com)
Lovenox: Injections used to help prevent micro-clotting associated with Thrombophelia and or auto-immune deficiencies (ivf.drcharlesmiller.com)
IVF/ICSI: refers to a procedure designed to overcome infertility and produce a pregnancy as a direct result of the intervention. In general, the ovaries are stimulated by a combination of fertility medications and then one or more oocyte(s) are aspirated from ovarian follicles. These are fertilized in the laboratory (“in vitro”), after which, one or more embryo(s) are transferred into the uterine cavity. These steps occur over about a two-week interval of time, which is called an IVF cycle. (ivf.drcharlesmiller.com)
Preimplantation Genetic Screening (PGS): performed on cell(s) removed from a preimplantation embryo or a polar body from an oocyte. The goal is to identify de-novo aneuploidy in embryo(s) of couples presumed to be chromosomally normal. Theoretically, avoiding transfer of aneuploid embryos will reduce the risk of pregnancy failure and improve the probability of conceiving a viable pregnancy (ivf.drcharlesmiller.com)
Lupron: injection given below the skin, subcutaneous injection. These medications are used to enable the body to produce a higher number of quality eggs. These medications are also designed to prevent the mid-cycle hormonal surge which can result in a cancelled cycle. (ivf.drcharlesmiller.com)
Menopur: (menotropins for injection) is a prescription medicine that contains hormones. MENOPUR contains follicle stimulating hormone and luteinizing hormone activity. These hormones stimulate healthy ovaries to make eggs. (Ferring Pharmaceuticals)
Follistim: medicine that contains follicle-stimulating hormone (FSH) to help healthy ovaries to develop (mature) and release eggs; and as part of treatment programs that use special techniques (skills) to help women get pregnant by causing their ovaries to produce more mature eggs (Merck)
*Please note that each patient's case is unique and Dr. Miller creates individual care plans for each couple based on their medical history. Not all patients who have the MTHFR gene mutation will be treated with Lovenox.